Stenosing ligamentitis disrupts the normal sliding of the tendon of the finger and gradually complicates the usual movements of the hand. The person first feels stiffness, then painful clicks appear, and in the later stages the finger is fixed in a bent position.
Today we will analyze the mechanism of development of the problem, typical causes, main symptoms, diagnostic principles and treatment approaches. After reading the article, you will learn when observation and conservative tactics are enough, and when doctors consider surgery.
In international sources, this condition is usually described as trigger finger or stenosing tenosynovitis. Its essence lies in the fact that the flexor tendon passes through the narrowed area of the tendon canal in the area of the A1 ring ligament (A1 pulley), so the movement becomes uneven and painful.
Clicking occurs when a thickened area of a tendon or its nodule passes through a dense canal with a mechanical obstacle. In everyday life, this condition is sometimes described as a crunchy finger. During its clinical evaluation, attention is paid to the blockage, soreness at the base of the finger and the nature of the motor restriction.
The problem is localized in the tendon area and its sheath, and not in the articular cartilage or ligaments. That is why the pain intensifies during movement, especially with flexion and subsequent extension.
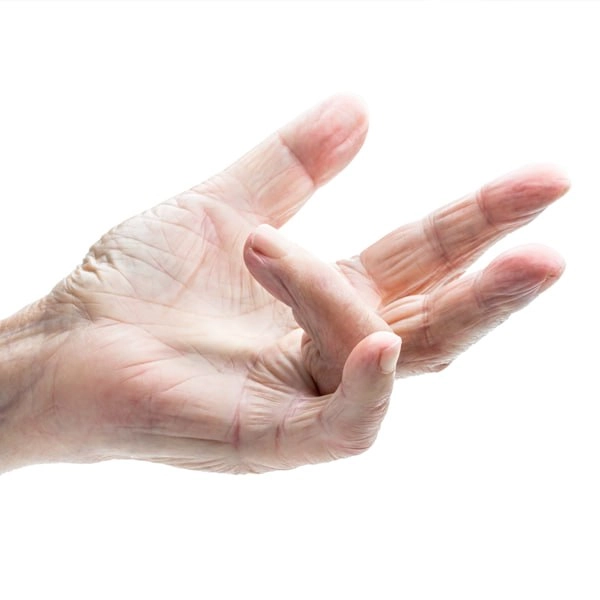
In modern clinical practice, repeated force movements of the hand, concomitant systemic diseases, older age and minor repetitive tendon injuries are singled out as the main risk factors.
The risk is increased by actions that require strong or prolonged engagement. These include:
In such conditions, the tendon rubs against the narrowed section of the canal. This supports irritation, local inflammation and subsequent thickening of the tissues, which causes the ligamentitis to progress faster.
Most often, doctors call diabetes mellitus and rheumatoid arthritis risk factors. In patients with such chronic diseases, the problem occurs more often, and the response to injectable and other conservative treatments may be weaker than in people without concomitant conditions.
If there is already a history of systemic inflammatory disease, the doctor assesses not only the finger itself, but also the general condition of the hand. This is necessary in order not to miss other sources of pain and stiffness that give a similar clinical picture.
Lesions are more often recorded in older people, especially after forty years. A separate role is played by microtraumas that accumulate gradually and do not always have one clear episode of damage in the anamnesis.
Due to repeated overload, the tendon sheath is irritated, and the tendon itself slips worse. Over time, this goes from early discomfort to a stable mechanical blocking of movement.
The clinical picture usually develops gradually. At first, the person feels uncomfortable during the first movements, and then pain, clicks and difficulties with full extension are added.
At the initial stage, complaints are not always sharp. More often there is morning stiffness, sensitivity in the palm of the hand at the base of the affected finger and the feeling that the movement is not quite free.
Early signs:
Such symptoms do not always interfere with household activities, but it is at this stage that the patient best notices the change in the usual movements of the hand.
Further, the symptoms become more pronounced. There is a painful click during movement, and the finger may suddenly linger in a bent position and extend only after additional effort with the second hand.
In more severe stages, the blockage is no longer episodic. In severe cases, described AAOS, the finger may not extend at all without the intervention of a medical specialist.
First, patients go to the family doctor, who evaluates the symptoms and selects the tactics for further action. If the problem does not go away, interferes with daily activities or progresses, the patient is usually examined by an orthopedic traumatologist, surgeon or other specialized specialist in hand pathology.
It is worth making an appointment with a doctor faster if:
This approach reduces the risk of persistent contracture, prolonged stiffness, and more difficult recovery after treatment.
In most cases, diagnosis is limited to examination. The doctor clarifies the complaints, the duration of the symptoms, the type of load on the hand, the presence of diabetes or rheumatoid process, and then evaluates the movement of the finger itself during the examination.
During the examination, the doctor looks for four basic signs:
It is this set of symptoms that in most cases allows us to draw a conclusion. The doctor also assesses whether complete passive and active extension is maintained. This is important because prolonged fixation of the finger affects the prognosis of mobility and the choice of further tactics.
In most cases, X-rays and MRI are not needed. A typical picture is often established already during a conversation and physical examination.
Ultrasound is used selectively when it is necessary to clarify the condition of the tendon, shell or exclude other pathology of the hand. In modern reviews, ultrasound is described as a useful tool to visualize ligament thickening, tendon nodules, and causes of blockage during movement.
Not every patient needs surgery. Initially, conservative treatment is usually considered: reducing the provocative load, night splinting, anesthesia, soft mobilization exercises and, according to indications, injection of a corticosteroid into the tendon canal area.
Surgical treatment is considered when conservative treatments do not provide adequate control of symptoms. A separate indication is the situation when the finger is already blocked in flexion and does not extend even after careful assistance with the second hand.
The main indications for the operation:
The essence of the intervention is to release the ligament and restore the free sliding of the tendon. This operation is usually performed on an outpatient basis under local anesthesia, through a small incision or with the help of other minimally invasive techniques.
After surgery, most patients are recommended to resume finger movements early. In the first days, pain, swelling in the palm and sensitivity in the incision area persist, and the complete disappearance of stiffness takes a few days longer than the skin to heal.
If the stiffness, swelling or pain lasts longer than expected, the doctor can connect physiotherapy. After surgery, it is important to follow the recommendations for dressings, loads and exercises, because this is what affects the return of the function of the hand.
Without treatment or with late treatment, the disease can turn into a persistent lock and prolonged stiffness of the finger. After surgery, there are also risks, although they are less common: it is infection, damage to the finger nerve, preservation of the click, pain in the scar or incomplete restoration of the extension.
To prevent relapse, it is important to reduce the repeated force load on the brush, to correct the work regime in time, and not to ignore morning stiffness or repeated episodes of blocking. In the presence of diabetes or rheumatoid inflammation, monitoring the concomitant condition together with a specialist doctor is of additional importance.
1100 UAH
Primary consultation of an orthopedist-traumatologist
900 UAH
Repeated consultation of the orthopedist-traumatologist
2100 UAH
Urgent consultation of an orthopedist-traumatologist
